Colposcopy
Colposcopy is a procedure that gives your health care provider a magnified view of your cervix. It's done using a lighted microscope called a colposcope. In most cases, a sample of cervical cells is taken during a biopsy. The sample can then be studied in a lab. If any problems are found, you and your provider will discuss treatment choices. It usually takes less than 30 minutes, and you can often go back to your normal routine right away.
Reasons for the procedure
Colposcopy is usually done as a follow-up exam to help find the cause of an abnormal Pap test. Results of an abnormal Pap test can mean that the cells don’t appear normal or that there are cancer cells. Abnormal cells can also be caused by infections. HPV (human papillomavirus) is a large family of viruses that can be passed from person to person through sex. HPV can cause genital warts. It can also cause changes in cervical cells. If an HPV test is positive and the Pap test is abnormal, a colposcopy may be recommended. Colposcopy is also used to evaluate other problems. These include:
-
Pain or bleeding during sex.
-
Postmenopausal bleeding.
-
Unexplained abnormal lower genital tract bleeding.
-
Sore (lesion) on the vulva or vagina.
-
Persistent abnormal vaginal discharge.
What are the risks?
Problems after colposcopy are very rare, but can include:
Getting ready for the procedure
Colposcopy is normally done in your health care provider’s office. It will be scheduled for a time when you’re not having your menstrual period. You may be asked to sign a form giving your consent to have the procedure. A day or two before the procedure, your provider may also ask you to:
-
Not have sex.
-
Stop using tampons.
-
Not use creams or other vaginal medicines.
-
Not clean out the vagina with water or other fluids (douche).
-
Take over-the-counter pain medicines an hour or two before the procedure.
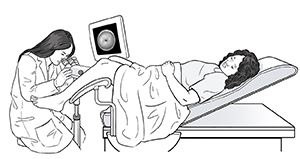
During colposcopy
-
You will be asked to lie on an exam table with your knees bent, just as you do for a Pap test.
-
A tool called a speculum is inserted into the vagina to hold it open.
-
A vinegar or iodine solution is applied to the cervix to make the abnormal cells easier to see. You may feel pressure or a slight burning for a few moments. In some cases, the cervix may be numbed first with an anesthetic.
-
The cervix is looked at through the colposcope. This is placed outside the vagina.
-
If your health care provider sees abnormal areas on your cervix, a biopsy will be done. You may feel a slight pinch and cramping. The tissue sample is sent to a lab for study.
-
An endocervical curettage may also be done at the time of colposcopy. In this procedure, a tool is put into the endocervical canal to get a sample of cells from the endocervix. This area can't be seen with a colposcope.
-
You may feel slight pinching or cramping during the biopsy. Medicine or a thick paste may be applied to the biopsy site to stop bleeding.
After the procedure
-
If you feel lightheaded or dizzy, you can rest on the table until you’re ready to sit up.
-
If a biopsy was done, you may have mild cramping or light bleeding for a few days. You may also have a thick, dark discharge from the medicine used to stop bleeding at the biopsy site.
-
Use pads or panty liners, but not tampons, for at least the first 24 hours.
-
If you have any discomfort, over-the-counter pain medicine can provide relief.
-
Ask your health care provider when you can have sex again.
Follow-up
If a biopsy was done, your health care provider will get the lab report in a week or 2. You and your provider can then discuss the results. In some cases, you may be scheduled for more tests or treatment. Be sure to keep follow-up appointments with your provider.
When to contact your doctor
Contact your health care provider if you have:
-
Heavy vaginal bleeding (more than one pad an hour for 2 hours).
-
Severe or increasing pelvic pain.
-
A fever over 100.4°F (38°C), or higher, or as directed by your provider.
-
Bad-smelling or unusual vaginal discharge.
Online Medical Reviewer:
Daphne Pierce-Smith RN MSN
Online Medical Reviewer:
Robyn Zercher FNP
Online Medical Reviewer:
Vinita Wadhawan Researcher
Date Last Reviewed:
2/1/2025
© 2000-2026 The StayWell Company, LLC. All rights reserved. This information is not intended as a substitute for professional medical care. Always follow your healthcare professional's instructions.